Rev Doc Watson
The promise of abundant life is fulfilled through optimizing our spiritual, physical, and mental health. The purpose of this blog is to share insights, information, and suggestions to help us all achieve this goal regardless of our age or circumstances.
Tuesday, April 16, 2024
Inpatient Psychiatric Hospital Closure
Saturday, March 16, 2024
The Heartbreaking Facts on Suicide
A recent piece in The Conversation (click here to view full article) has spotlighted concerning statistics on suicide, shedding light on a pressing issue that demands attention. In 2021, the CDC reported a distressing reality: every 11 minutes, someone in the US took their own life, resulting in nearly 50,000 deaths annually. Furthermore, 1.7 million individuals attempted suicide, with over 12 million grappling with suicidal thoughts. These figures translate to approximately 3.6% of the US population in 2021 experiencing such thoughts.
Tragically, the numbers took a somber turn in 2022, with suicides increasing by 2.6%. Alarmingly, suicide remains one of the top three causes of death for individuals aged 10 to 34, underscoring the urgent need for a reassessment of our suicide prevention strategies.
My personal journey, marked by the loss of a loved one to suicide, ignited my path towards psychiatry. This experience continues to be the driving force behind my commitment to this field. I envision a world where the very notion of suicide is foreign to us. Yet, in my practice, I encounter individuals trapped in the grips of depression, consumed by a sense of hopelessness. They struggle to envision a future beyond their current despair, unable to fathom the possibility of emerging into the light of joy, happiness, and fulfillment.
If you find yourself wrestling with depression or suicidal thoughts, please reach out for help. Share your burden with a friend, a family member, a healthcare professional, or anyone you trust. While the path to recovery may seem obscured by darkness, know that it does exist. I witness this transformation firsthand in my patients, as they navigate their way out of the abyss. Even those who have attempted suicide express gratitude for having survived.
If you are contemplating self-harm or suicide, seek assistance immediately:
- Call 911 for emergency services.
- Visit the nearest hospital emergency room for evaluation and possible admission for your safety.
- Reach out to the Suicide and Crisis Lifeline by calling or texting 988.
Monday, April 25, 2022
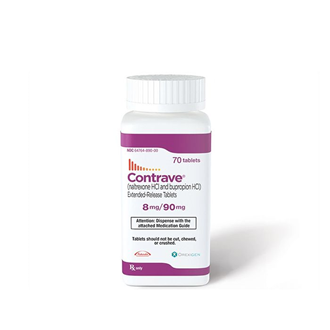
Having a hard time losing those extra COVID pounds? Consider CONTRAVE…
The American Psychological Association released a study
conducted in February 2021 that showed that 42% of Americans gained more weight
than they intended since the start of the pandemic. Average weight gain was 29
pounds, with 10% reporting that they gained more than 50 pounds.
Diet and exercise are of course the best ways to approach a
return to a healthy weight. But if you’ve
been trying and diet and exercise alone just isn’t working for you, I wanted to
share information about a non-stimulant, non-controlled substance weight loss
medication. It’s called Contrave, and many of my patients have reported a good
response.
Contrave is a combination of two medications, bupropion (Wellbutrin)
and naltrexone. Together, these two medications work on the hypothalamus and
the mesolimbic circuit in the brain to reduce hunger AND reduce cravings. In clinical
studies, the average percentage weight loss with Contrave was 5.4% of body
weight (or about 12 pounds).
It is generally well tolerated, but common side effects
include:
·
Nausea
·
Constipation and other GI side effects
·
Headache
·
Trouble sleeping
·
Dry mouth
There are also serious side effects, especially in people
who have a history of seizures or use opioid medications.
As with any medication, you should speak with your doctor before
starting Contrave to see if it is a good (and safe) choice for you.
For more information visit the Cotrave web site by clicking HERE.
There are coupons available (insurance usually doesn’t cover the cost) and much
more information.
Saturday, January 15, 2022
Love your neighbor...with some carrot cake
As COVID continues to take its
toll on our psyche, we could all do with a few more bright moments in our
lives. Towards that end, I'm sharing our family recipe for carrot cake. I'm not
quite sure where it came from, probably from my grandmother who loved to clip recipes from
the LA Times. It is hands down one of the best carrot cakes I've ever
tasted. Why not make one and leave a few pieces at a neighbor or friends’ door
and spread some cheer...
Ingredients:
Cake:
2 cups flour
2 teaspoons baking powder
1 1/2 teaspoons baking soda
1 teaspoon salt
2 teaspoons cinnamon
4 eggs
2 cups sugar
1 1/2 cups oil
2 cups grated carrots
about 8 ounces crushed
pineapple, juice drained
1/2 cup walnuts or pecans
Vanilla Cream Cheese Frosting:
1/2 cup butter
8 ounces cream cheese
1 teaspoon vanilla
1-pound powdered sugar
Instructions:
Preheat oven to 350
degrees.
Beat together the eggs and sugar,
let it stand for a while, at least 5 minutes, for the sugar to dissolve.
Mix dry ingredients: flour,
baking powder, soda, salt, and cinnamon.
Stir oil, carrots, drained
pineapple, and nuts into the egg and sugar mixture.
Add the dry ingredients and mix.
Grease and flour a 13x9 inch
pan (could probably use round pans and make a layered cake but you’d need to
decrease the baking time). Put cake batter in pan. Bake for approx. 55 min--I
start checking around 50 min. It is done when it springs back when lightly
touched. Remove from oven and cool.
While cake cools, make the
frosting. Mix together the butter, cream cheese, vanilla, and powdered sugar.
Once the cake is completely cool, spread on the frosting.
Enjoy!
Saturday, June 12, 2021
Covid isolation made me forget how to be human: dealing with the anxiety of our return to "normal"
We’ve reached the point where the US is relaxing its
COVID-19 precautions. That cases have fallen to the point that this is possible
is incredibly good news, the answer to prayer, and a source of great joy.
However, I am also seeing a spike in anxiety in my outpatient psychiatric practice.
As I recently heard someone say, “it’s like I’ve forgotten how to be human.”
Although the person was joking, there is some truth to the
comment. Many of us have been isolated for the last 15+ months. Social
interactions have been online, or with masked strangers on the occasional
essential trip out of the house. If we interacted with others in person, it was
only with a select few and usually with people we knew very well. Or we were
essential workers living with the stress of the unknown—would we catch the
virus? If so, how severe would our case be? Were we exposing our loved ones and
family due to our work? Many of us have lost loved ones, and the threat of
death was present everywhere. Some people faced their own mortality and the
mortality of those they love for the first time. It has been a very difficult and stressful
time.
Many people live with diagnosable anxiety disorders. These
include:
·
social anxiety: marked fear or anxiety about one
or more social situations in which the individual is exposed to possible
scrutiny by others
·
generalized
anxiety disorder: excessive anxiety and worry, an “apprehensive expectation” about
a number of events or activities
·
panic disorder: an abrupt surge of intense fear
or discomfort that reaches a peak in minutes during which physical and
cognitive symptoms occur
·
agoraphobia: intense fear or anxiety triggered
by the real or anticipated exposure to a wide range of situations
For some people who lived with an anxiety disorder prior to the
pandemic-imposed isolation, returning to “normal” life can be extremely
stressful. Many people who live with these disorders described a feeling of relief
that they did not have to be out in the world during the pandemic, and that
they could interact with others free of some of the stressors that induced
symptoms.
But even if a person does not live with a diagnosable
anxiety disorder, returning to “normal” life can still be hard. Some people
remain fearful of interactions due to safety concerns. Is it okay to interact
with others without a mask? Is that person really vaccinated? What about my
children (or grandchildren) who aren’t eligible for the vaccine? Will it
be safe to return to work in person? For others, it is that we are out of the
habit of interacting with others. We are used to being around our homes, and we
have forgotten how to interact with others in person.
So how do we cope? One way is to take comfort in the fact
that we are not alone if we experience fear and discomfort in social situations.
If you are feeling a little uneasy about being back out in the real world, chances
are that those around you are too. It is a time for us to be especially gentle
and understanding with one another.
Another way to manage is to remember some of the coping
mechanisms that we developed during the pandemic to handle stress. Many people
found solace in new, calming activities: cooking, gardening, playing chess,
virtual yoga and workouts, writing real letters on paper to others, walking/hiking
and more. We can take these activities with us as new ways to cope with our
anxiety and worry as life begins to return to normal.
And we can pray, and take comfort in God’s word as found in
Isaiah 41:10:
Do not fear, for
I am with you,
do not be afraid, for I am your God;
I will strengthen you, I will
help you,
I will uphold you with my victorious
right hand. (NRSV)
However, some people may need professional help. If your anxiety
or worry is causing you significant distress or impairment in social, occupational,
or other important areas of functioning, it is time to reach out. You can start
by talking to your primary care doctor who can assist or refer you to a mental
health professional for therapy or medication if indicated.
This has been a very difficult year filled with loss, fear,
and isolation. As we begin to emerge from the darkness of this time, we can
remember that anxiety is normal given what we have all been through. In fact,
it is very “human.”
This article originally appeared in the weekly newsletter of the Episcopal Diocese of San Diego
Monday, April 5, 2021
A recent article in the Journal of Addiction Medicine
reported on changes in alcohol consumption in response to the COVID-19
pandemic in the United States. The researchers found that during the pandemic
there has been a 29% increase in the number of alcoholic drinks that people are
consuming, a 20% increase in those exceeding the recommended drinking limits,
and a 21% increase in binge drinking. Among the researchers conclusions is that
there is an association among the COVID-19 pandemic and the amount of alcohol
consumption and that public health monitoring is warranted.[i]
If you have found yourself drinking more during the pandemic, you are not alone. Here are ten questions to ask yourself to help you determine if your drinking may have become harmful:
1 How
often do you have a drink containing alcohol? Never/Monthly or less/2-4 times a
month/2-3 times a week/4 or more times a week (A drink is defined as 12 ounces of beer, 8-9 ounces of malt liquor, 5
ounces of wine, or 1.5 ounces of 80-proof hard liquor)
2.
How many drinks containing alcohol do you have
on a typical day when you are drinking? 1-2/3-4/5-6/7-9/10 or more
3.
How often do you have 6 or more drinks on one
occasion? Never/Less than monthly/Monthly/Weekly/Daily or almost daily
4.
How often during the last year have you found
that you were not able to stop drinking once you had started? Never/Less than
monthly/Monthly/Weekly/Daily or almost daily
5.
How often during the last year have you failed
to do what was normally expected from you because of drinking? Never/Less than
monthly/Monthly/Weekly/Daily or almost daily
6.
How often during the last year have you needed a
first drink in the morning to get yourself going after a heavy drinking
session? Never/Less than monthly/Monthly/Weekly/Daily or almost daily
7.
How often during the last year have you had a
feeling of guilt or remorse after drinking? Never/Less than
monthly/Monthly/Weekly/Daily or almost daily
8.
How often during the last year have you been
unable to remember what happened the night before because you had been
drinking? Never/Less than monthly/Monthly/Weekly/Daily or almost daily
9. Have you or someone else been injured as a
result of your drinking? Never/Yes, but not in the last year/Yes during the
last year
10 Has a relative, or friend, or a doctor or other
health worker been concerned about your drinking or suggested you cut down? ?
Never/Yes, but not in the last year/Yes during the last year
Scoring:
Item 1: Never=0/Monthly or less=1/2-4 times a month=2/2-3
times a week=3/4 or more times a week=4
Item 2: 1-2=0/3-4=1/5-6=2/7-9=3/10 or more=4
Items 3-8: Never=0/Less than
monthly=1/Monthly=2/Weekly=3/Daily or almost daily=4
Items 9-10:
Never=0/Yes, but not in the last year=2/Yes during the last year=4
If you scored above 8, or even if you didn’t but feel that you sometimes drink too much alcohol, or that your drinking is causing problems, or your family is concerned about your drinking, talk to your clergy person or your doctor. They can help you determine if you need to cut back or quit altogether, and steer you in the right direction.
Some resources for you also might consider are:
·
Alcoholics Anonymous (national site): CLICK HERE
·
Dry January (tools and information about taking
a one month break from drinking--it can be any month, not just January): CLICK HERE
·
Consider reading: Quit Like a woman: The Radical Choice to Not Drink in a Culture
Obsessed with Alcohol by Holly Whitaker
We close with the full version of the Serenity Prayer attributed to Reinhold Niebuhr (a shortened version is used in many 12-step programs):
God grant me the serenity
To accept the things I cannot change;
Courage to change the things I can;
And wisdom to know the difference.
Living one day at a time;
Enjoying one moment at a time;
Accepting hardships as the pathway to peace;
Taking, as He did, this sinful world
As it is, not as I would have it;
Trusting that He will make things right
If I surrender to His Will;
So that I may be reasonably happy in this life
And supremely happy with Him
Forever and ever in the next.
Amen.
I Barbosa, C., Cowell,
A. J., & Dowd, W. N. (2020). Alcohol consumption in response to the
COVID-19 pandemic in the United States. Journal of Addiction Medicine. https://doi.org/10.1097/adm.0000000000000767
Thursday, March 25, 2021
After a Suicide...
If you are considering suicide, seek help immediately. Call 911 or the National Suicide Prevention Lifeline at 1-800-273-TALK (8255). There is also a Crisis Text Line: Text HOME to 741741. For crisis support in Spanish, call 1-888-628-9454.
Two Sundays ago I had the privilege of speaking at a forum in a congregation that had just experienced the loss of a member by suicide. While mental health struggles are always common in the US, with COVID we are seeing a rise in depression, anxiety, PTSD, substance use, and insomnia. Over the coming weeks, I will be addressing mental health concerns as we all strive to maintain our mental, physical, and spiritual health in these trying times. In the past I've posted on what to do if you or someone you know is considering suicide. Today, I'm sharing some tips for what to do in the aftermath of a completed suicide.
It can be hard to know how to help someone whose life has been impacted by suicide. Knowing what to say, and what not to say, is important. Specifically:
- Avoid clichés about God’s plan, or God’s need for another angel in heaven
- Do NOT ask for the specifics about the death
- Do not assume the person who completed suicide, or the survivor(s), were/are angry
- Do not assume the survivor(s) are guilty
- Avoid saying, “God never gives us more than we can handle” to the grieving survivors
- Avoid saying “I know how you feel”. Really none of us ever really knows exactly how another feels. We can experience similar losses, but the impact and experience is never exactly the same. Instead you can consider saying, “I don’t know what to say, I have no idea what you’re going through, but I care about you and I want to be here for you.”
- Avoid saying, “I can’t imagine”. This can make the survivor feel even more isolated.
- Avoid saying, “Let me know if I can help”. It is hard for people to ask for help in even the best of circumstances, and following a suicide it is even harder. Instead do something specific for the survivors, like shop for groceries, bring dinner, etc.
- Be cautious when saying “I’ll be praying for you.” If this is truly your commitment, is heartfelt and you are going to follow through then it is a welcome message that can be comforting. But if insincere, or used as filler when you don’t really know what to say, it can feel dismissive.
- Do not assume your theology about suicide is the same as the survivors.
There are also tangible things that you can do following a suicide. Specifically, you can:
- Organize a team in the person’s name to walk in the next AFSP walk in San Diego (Out of the Darkness Walks—Overnight and Day) https://www.theovernight.org/index.cfm?fuseaction=cms.page&id=1359&eventID=518
- Consider starting a scholarship fund for education in lieu of flowers if the person had children—assist the survivors by setting this up at a local bank for the family or as a GoFundMe page.
- Read about suicide loss (AFPS site has a list of resources: https://afsp.org/books-for-loss-survivors )
- Assist those touched by the suicide to connect with other suicide survivors (AFSP has a Healing Conversations program and bereavement support groups. You can offer to accompany them to an event or sit with them if it is online so that they don’t feel so alone. https://afsp.org/healing-conversations )
- Encourage counseling/seeking mental health help.
- Just be there (walking, watching a movie, etc)
- Be patient. Months after the event are often the most difficult. Continue to check in, let them know you are thinking of them, that you’re there for them, and that you want to list.
- Remind survivors of the importance of self-care—rest, eating well, excercise
I close with a prayer written by The Rev. Talitha Arnold for the National Action Alliance for Suicide Prevention:
God of all mercy, from whose love nothing can separate us, we pray this day for all persons dealing with mental illness and those who love and care for them. Especially this day, we pray for all whose lives have been touched by suicide, for those who have died by suicide and those who have attempted it. We pray for those who, because of mental health challenges such as depression, PTSD, or bipolar disorder, live with thoughts of suicide. We pray for those who live in despair and without hope because of poverty or discrimination. We pray for families and friends, colleagues and co-workers, who have been touched by the suicide of a loved one. We pray for counselors and therapists, psychologists and psychiatrists, for pastors, rabbis, priests, and imams, and for all who seek to help. And we pray, too, that you might give us the courage and wisdom to be there for others in distress, to offer your love and our care, to help break the silence and change the conversation about suicide, to be your listening ear, your hands, and your heart for others. Amen.
The above lists of suggestions come from a variety of sources, including those from the insightful members of a congregation that suffered the loss of one of their community by suicide, the American Foundation for Suicide Prevention website, and my own experience following the death of my spouse. This article was originally written for and published by The Episcopal Diocese of San Diego.